Periodontitis, more commonly known as gum disease, is a serious gum infection that damages the soft tissue and destroys the bone supporting your teeth. It is a progressive condition, which, if left untreated, can lead to tooth loss and impact your overall health.
Around 22.9% of the Australian population is estimated to have periodontitis. The prevalence of periodontitis tends to rise with age, with the highest rate of 60.8% observed among individuals above 75 and the male population showing a slightly higher prevalence.
Even though gum disease is mostly preventable, most people may be unaware that they have this condition. With the age-old adage, prevention is better than cure, never being more accurate, it’s essential to understand this serious oral disease and take the necessary steps to reduce and prevent its risk. In this blog, we’ll provide a comprehensive guide to help you understand gum disease, its causes, risks, symptoms, and periodontitis prevention and treatment.
Understanding Periodontitis
Periodontitis develops and progresses through a series of stages. It begins with the accumulation of plaque and bacteria on the teeth and along the gum line. If the plaque buildup is not removed through proper oral hygiene and professional treatment routinely, the bacteria in plaque release toxins that trigger an inflammatory response in the gums. This leads to the first stage of gum disease, gingivitis.
When the plaque hardens, it turns into tartar which can settle near and into the gum line. The bacterial toxins then harm the teeth structure, leading to inflammation and deterioration of the gum tissue, causing the gums to pull away from the teeth and create spaces called periodontal pockets. These pockets provide a favourable environment for more bacteria to thrive, leading to further infection. The disease progression can cause a breakdown of the connective tissue and bone supporting the teeth, leading to gum recession, bone loss, and loosening of the teeth.
Symptoms of Gum Disease
Gum disease is typically a silent and painless disease, with minor symptoms. These symptoms may not be necessary because of gum disease and may be due to other oral health issues. This is why it’s vital to visit the dentist to identify the underlying cause and get appropriate treatment. A dentist can help identify the root cause of any oral problem for early treatment to prevent gum disease or oral conditions.
Some of the symptoms of gum disease include:
- Red, swollen, or tender gums
- Bleeding gums, especially during brushing or flossing
- Gum recession which also makes the teeth appear longer
- Persistent bad breath or a foul taste in the mouth
- Formation of deep pockets between the teeth and gums
- Loose or shifting teeth
- Changes in the bite or the way teeth fit together
- Changes in the fit of dentures or other dental appliances
- Pus between the teeth and gums
- Changes in the appearance of the gums, such as shiny or dusky appearance
Stages of Gum Disease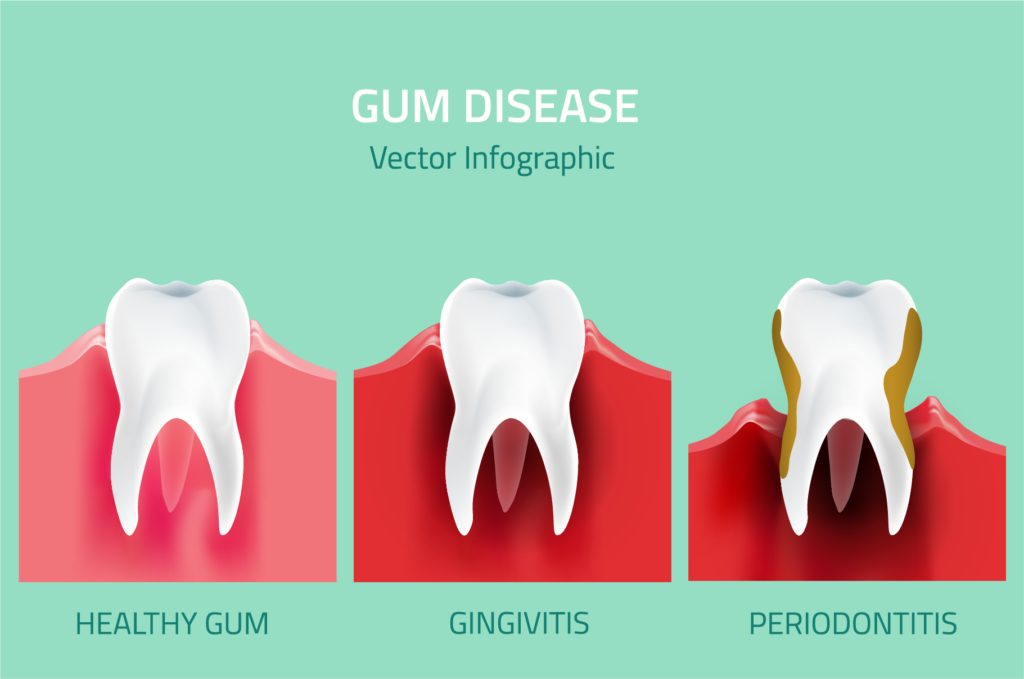
Periodontitis progresses through different stages, each characterised by specific changes and severity of the condition. The stages include:
Gingivitis
Swollen and inflamed gums that bleed easily are usually an indication of the earliest form of gum disease, gingivitis. The gums can get inflamed because of the plaque buildup on the teeth and around the gum line, making them appear red and swollen. However, at this stage, the bone and connective tissues are still unaffected and removing the plaque through a professional cleaning can help stop the progression.
Early Periodontitis
As gingivitis progresses, it can develop into early periodontitis. The infection begins to spread below the gum line, causing the gums to recede and form periodontal pockets. Some bone loss may begin to occur, and symptoms such as bad breath and gum sensitivity may become more noticeable.
Moderate Periodontitis
As the infection advances, it causes further damage to the gum tissue, bone, and fibres that hold the teeth in place. The pockets become deeper, and the bone loss becomes more significant. Teeth may become loose, and there may be increased tooth sensitivity and pain while chewing.
Advanced Periodontitis
At the advanced stage, there is severe damage to the supporting structures around the teeth, the infection has spread, and you can see visible signs of the disease, such as loose teeth and abscesses with severe discomfort.
Causes & Risk Factors
Some of the causes and risk factors of gum disease include:
Plaque and Tartar Buildup
Plaque is a sticky film composed of bacteria, food particles, and saliva that constantly forms on the teeth. If plaque is not regularly removed through brushing and flossing, it can harden and become tartar (calculus). Tartar is more difficult to remove and acts as a reservoir for bacteria, leading to an increased risk of periodontal infection.
Poor Oral Hygiene
Poor oral hygiene habits, such as infrequent or inadequate brushing and flossing, contribute to the accumulation of plaque and bacteria in the mouth. It’s recommended to brush twice daily with strong fluoride toothpaste, floss regularly to remove the food particles between the teeth and use antibacterial toothpaste to maintain oral hygiene.
Systemic Diseases
Certain systemic diseases and conditions can increase the risk of developing periodontitis. Diabetes, for example, can negatively affect the body’s ability to control blood sugar levels and fight infections. Individuals with diabetes are more prone to gum disease and may experience more severe forms of periodontitis. Other systemic conditions, such as cardiovascular and respiratory diseases, have also been linked to an increased risk of periodontitis.
Lifestyle
Lifestyle choices can impact the health of the gums and increase the risk of periodontitis. Smoking reduces blood flow to the gums, and impairs the immune system’s response, hampering the healing process. Poor nutrition, obesity, and foods high in sugar also increase the risk of gum disease and tooth decay.
Hormonal Changes
Hormonal fluctuations in women, such as those occurring during puberty, pregnancy, and menopause, can affect the gum’s response to plaque and increase the risk of gum disease. Hormonal changes can lead to increased blood flow and sensitivity in the gums, making them more susceptible to inflammation and infection.
Weakened Immune System
Individuals with a weakened immune system are more susceptible to infections. Conditions that compromise the immune system, such as cancer, and autoimmune disorders, can impair the body’s ability to fight off bacteria and control inflammation. This makes the gums more vulnerable to periodontal infections and can accelerate the progression of periodontitis.
It’s important to note that while these factors increase the risk of developing periodontitis, their presence does not guarantee the development of the disease. Maintaining good oral hygiene practices, regular dental checkups, and adopting a healthy lifestyle can help reduce the risk and severity of periodontitis.
Gum Disease Prevention
Gum disease develops in stages, with the initial stages being easily preventable with good oral hygiene, a balanced diet, and a healthy lifestyle. But as the disease progresses, treatment is necessary to prevent tooth, bone and gum loss and serious health risks. Prevention is the key, and early detection is critical to minimise further damage and lengthier treatment times.
Gum Disease Treatments
Gum disease treatment may vary depending on the stage of your periodontitis, teeth conditions and overall health. Mild gingivitis, or the initial stage of gum disease may require only a single procedure, whereas advanced periodontitis may need more extensive treatment.
Some of the treatments for gum disease include:
Non-Surgical Treatments
A deep cleaning procedure with scaling and root planing can remove plaque or tartar buildup. It involves using special dental tools to scrape plaque or tartar from around and in between teeth surfaces and the gum line. Sometimes, antibiotics may be prescribed to control infection and reduce bacterial growth. After treatment, it is vital to maintain your oral health with good oral hygiene and regular dental checkups to prevent relapse.
Surgical Treatments
Advanced periodontitis may require surgical treatments to restore bone loss and promote gum healing. Flap surgery and bone and soft tissue grafts can help treat the more serious problems related to bone loss for improved oral health and regeneration of bone, gums, and soft mouth tissues.
Role of Dentists in Preventing Periodontitis
Dentists play a critical role in preventing periodontitis by conducting general checkups, performing deep cleaning procedures, providing oral hygiene guidance, and offering early treatment and intervention. Regular visits to the dentist allow for early detection, intervention, and monitoring of gum health, ultimately contributing to the prevention and management of periodontitis. It is important to maintain a collaborative relationship with your dentist to ensure proactive oral health care and the prevention of periodontal disease.
Some of the ways a dentist can help prevent periodontitis and achieve optimal oral health include:
General Checkups
Dentists can detect early signs of gum disease by monitoring your oral health to identify potential or emerging issues. During checkups, dentists examine the gums, teeth, and surrounding structures, looking for signs of inflammation, bleeding, pocket formation, and bone loss. By identifying these signs early on, dentists can intervene promptly and prevent the progression of periodontitis.
Routine checkups also help identify early signs of tooth decay, impacted wisdom teeth and other oral issues for early treatment, reducing the need for extensive dental procedures.
Deep Cleaning
Deep cleaning procedures, such as scaling and root planing are part of regular dental checkups. This prevents bacterial accumulation in your mouth, helping eliminate bacteria and toxins that cause gum inflammation and tooth decay.
Oral Hygiene Guidance
Dentists provide valuable guidance on proper oral hygiene practices to prevent periodontitis. This allows you to learn the correct techniques for brushing and flossing and maintenance of your teeth and gums.
At Superior Smiles, we offer personalised hygiene treatment plans, listening and understanding your concerns to help improve your health. Our caring dentists provide valuable oral hygiene education and tips, recommendation of age and dental condition-appropriate products and use the latest dental technology for superior hygiene, such as Airflow Therapy for a gentle, whole mouth clean.
Early Treatment & Intervention
Dentists play a pivotal role in early treatment and intervention of oral diseases. Oral examinations, x-rays and comprehensive consultations allow our Fremantle dentists to recognise the early signs of gum disease and minimise the risk of it progressing into a more advanced stage. We also evaluate the severity of periodontitis and develop bespoke treatment plans to manage the condition with tailored treatments.
Oral Hygiene and Its Impact on Periodontitis Prevention
Maintaining good oral hygiene, using appropriate dental products, staying up-to-date with regular dental checkups, and demonstrating consistency in oral hygiene practices are crucial elements in the prevention of various oral health issues, particularly gum disease. By prioritising oral hygiene, you can effectively combat the accumulation of plaque and bacteria, safeguarding your teeth and gums.
Preventive Dental Care is the Foundation of Optimal & Lasting Oral Health.
At Superior Smiles, prevention forms the core of our dental philosophy and care. We believe maintenance, accurate diagnosis and early treatment are the building blocks for a lasting and healthy smile. With a holistic approach and dedication to help you achieve optimal oral health, we’re here to help you on your oral health journey. Book a consultation to learn more about periodontitis prevention and treatment today.